How Much Do Family Nurse Practitioners Make?
Family nurse practitioners provide many of the same services as [...]
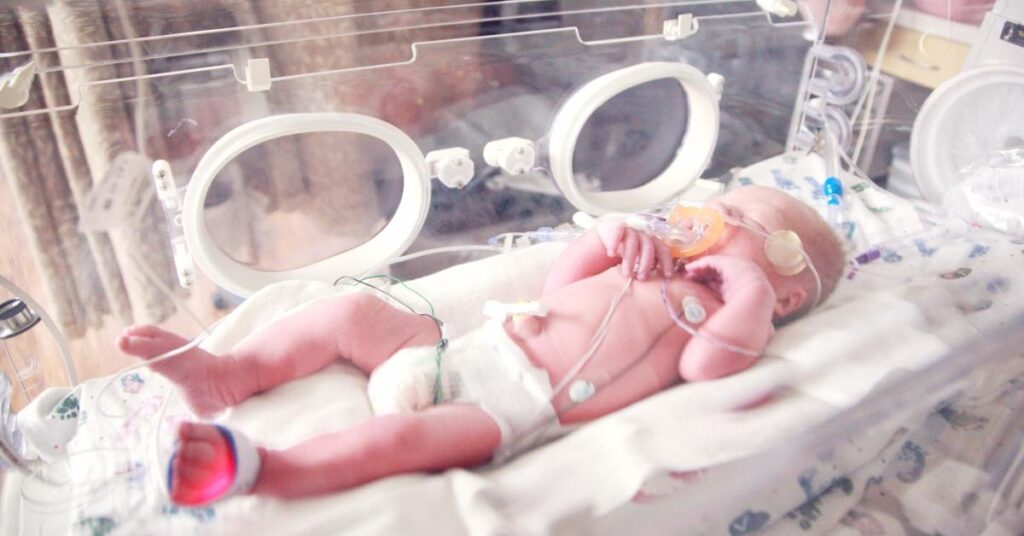
Neonatal nursing serves a most vulnerable population: newborn infants. Timely and effective care for these tiny children can impact their long-term health and viability immeasurably, particularly when something goes awry with a pregnancy, such as premature birth, disabilities and malformations, or infection or other maladies.
Neonatal nurse practitioners are the advanced practice nurses who tend to these defenseless newborns. They practice in delivery wards, emergency rooms, and neonatal intensive care units and other medical centers, typically under high-pressure conditions. As the president of the Council of International Neonatal Nurses, Inc. (COINN) Dr. Karen Walker observed: “For a neonatal nurse, a miscalculation in medications by even a minute amount in a 600g baby can make the difference between life and death or permanent disability. Never are we ‘just a nurse.'”
If you’re considering a career in neonatology, you may be wondering what training you’ll need to qualify. You probably also wonder how much do neonatal nurse practitioners make? This article addresses those questions, discussing:
Nearly 10,000 babies are born in the United States every day. The vast majority of these births are relatively uneventful. However, about one in ten infants are born preterm; about one in twelve has a low birthweight. Others manifest malformations or diseases that require special care.
Neonatal nurse practitioners (NNP) treat these special cases. Neonatal nurses typically work in hospital settings, providing treatment to premature and ill newborns. Some of these children must be admitted to the neonatal intensive care unit (NICU), where they may require specialized care for several months.
Nurse practitioners are highly trained nursing specialists who hold a Master of Science in Nursing degree. Over 350,000 are licensed to practice in the United States, approximately 1,800 of whom practice neonatal nursing (family medicine is the top nurse practitioner field, claiming nearly two-thirds of NPs; adult-gerontology primary care ranks second with about 9 percent of all NPs). They hold specialized licenses to practice in their field of expertise.
Nurse practitioners fulfill many responsibilities, including:
Neonatal nurse practitioners typically work with infants facing medical and surgical challenges immediately after birth. They provide standard daily care, including bathing, feeding, and changing diapers. They also administer more specialized care, including tube feedings, medication administration, blood transfusions, and intravenous fluids. They care for high-risk infants who may experience low birth weights, heart abnormalities, infections, and other health issues.
In addition, NNPs perform comprehensive assessments and screenings, including oxygen levels, vital signs, fluid intake, and hearing and vision tests. They maintain detailed records and engage with parents and care providers to disclose the infant’s status and provide support and education. Neonatal nurse practitioners also sometimes respond to neonatal emergencies in labor and delivery units.
NNPs can work with several infants at a time. Their patients typically require round-the-clock healthcare, including weekends and holidays. As such, NNPs can expect to work 12-hour shifts, though some workplaces accommodate eight to 10-hour shifts.
Did you know that anemia, arrhythmias, and acute respiratory lower infection are the top diagnoses that NNPs treat? Check out these four additional facts:
Maurice has always held a passion for working with infants. He works as a full-time neonatal nurse practitioner at the Children’s Hospital of Philadelphia (CHOP). Each day, he attends to the needs of three newborns in the neonatal intensive care unit.
One of his patients, Jamal, was born with a rare genetic condition involving chromosomal duplication. Maurice is one of a six-person team dedicated to Jamal’s daily care. To start the morning, the team meets to coordinate care plans for the day. Maurice is tasked with monitoring Jamal’s fluids. Today, he removes 160 cubic centimeters of excess fluid in Jamal’s abdomen and around his lungs. Maurice notices a measurable improvement in Jamal’s oxygen levels once the fluid is removed.
Maurice also ensures that Jamal receives the necessary nutrients and medications through his breathing tube and IV. Maurice and his coworkers run labs every six hours to monitor Jamal’s electrolytes and gasses. Throughout his day, Maurice records his observations and notes in Jamal’s charts to keep everyone abreast of his progress. Before Maurice’s shift ends, he administers a blood transfusion to Jamal due to anemia. Jamal tolerates it well, and his blood pressure improves.
Watching infants make daily progress is encouraging and rewarding. Maurice concludes his day feeling he’s truly made a difference in the lives of Jamal and his parents.
According to Glassdoor user data, the estimated total pay for a neonatal nurse practitioner in the United States is almost $118,000 in total compensation, including salary (approximately $111,000) and incentives (approximately $7,000). Top paying employers in the United States include Pediatrix, Texas Children’s Hospital, and Mount Carmel Health.
According to ZipRecruiter, NNPs in the state of Washington earn the highest average salaries (almost $131,000), followed by New York ($123,000), California ($118,000), and Idaho ($117,000). The lowest-paying states include North Carolina ($80,000), Louisiana ($84,000), Georgia ($86,000), and Illinois ($89,000).
Neonatal nurse practitioners require extensive training and hands-on experience to excel at their professions.
The first step in becoming a neonatal nurse practitioner is to earn your registered nursing credentials. You can do this by obtaining a bachelor’s degree in nursing (BSN), an associate’s degree in nursing, or a diploma from a hospital-based nursing school. If you choose the associate’s degree or diploma, you will eventually have to complete bachelor’s-level prerequisites before you can enroll in a Master of Science in Nursing program.
Once you meet the eligibility requirements for state licensure, you must sit for and pass the National Council Licensure Examination for Registered Nursest (NCLEX) exam to earn your RN license.
In addition to their RN license, NNPs must also hold a higher degree, such as a master’s degree or a Doctor of Nursing practice from an accredited program with a specialty in neonatal nursing. Earning these degrees will enable you to provide primary care to patients.
NNP program curricula may include advanced pharmacology, high-risk neonate theory, pediatric physiologic development, and advanced pathophysiology. Degrees can be completed either in-person or online. They include:
You may also pursue a post-graduate certificate if your graduate degree differs from the specialty area you wish to pursue as a nurse practitioner. Enrollment requirements typically include an MSN or a nurse practitioner qualification in another specialty.
In order to gain acceptance into an MSN or DNP graduate program, you’ll likely need at least one year of experience in a neonatal intensive care unit or comparable clinical experience. Requirements vary by school and specialty area.
Neonatal nurses must earn an MSN or DNP. They must also qualify for licensure; requirements vary by state. Applicants typically need to hold a master’s degree from an accredited nursing education program, pass the NCLEX-RN exam, and pass a background check. States may also require nurses to complete a minimum number of continuing patient contact hours and continuing education requirements.
With a Master of Science in Nursing (MSN) or a Doctor of Nursing Practice (DNP), nurse practitioners can pursue clinical leadership roles in managing the healthcare needs of infants. They can oversee ventilators, order diagnostic tests, and even perform heart catheterizations on pediatric patients. Healthcare organizations may give preference to nurse practitioners over registered nurses when hiring for neonatal nursing roles because their qualifications make them more versatile and thus more valuable.
The NCSBN website maintains links to each state’s testing and licensure requirements.
NNPs may also choose to obtain various certifications to increase their competitive advantage and validate their skills. The following organizations offer relevant credentials:
Being a neonatal nurse practitioner offers professionals the chance to undertake rewarding work while earning a competitive salary. Even though the job can be challenging and emotionally taxing, NNPs help newborns and their families through some of the most difficult times they’ll face, enabling severely ill patients to recover and thrive.
.
Questions or feedback? Email editor@noodle.com

Family nurse practitioners provide many of the same services as [...]

You need to have an RN license and have several [...]

Many hospitals experiencing COVID case surges offer nurses short-term positions [...]

Choosing a PMHNP program can be difficult. Much depends on [...]

The clinical practicum is essential to every psychiatric mental health [...]
Categorized as: Nurse Practitioner, Nursing & Healthcare