
Jobs in Industrial Engineering
Industrial engineers use fundamental skills transferable to systems and management [...]
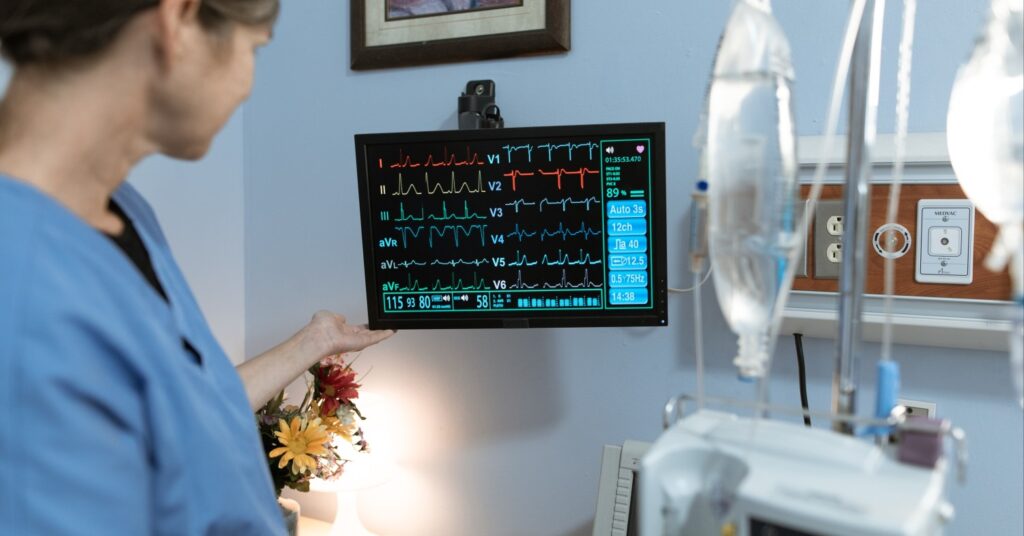
Health informatics (HI), an emerging healthcare discipline that combines big data and medical practice, utilizes health information technology (IT) systems to analyze patient data and devise improved solutions. Health informatics professionals, also known as informaticians, use data in beneficial ways to improve healthcare delivery, reduce costs related to healthcare, curtail errors, and identify public health trends.
Alongside the benefits it facilitates, big data also pses genuine risks. Health information aggregation simplifies access to patient data by storing it in a centralized infrastructure, raising obvious concerns about privacy and related issues.
As the old adage cautions, with great power comes great responsibility. It’s one reason informatics professionals must adhere to a strict ethical code to ensure patient privacy and confidentiality. In this article, we’ll summarize ethical issues in health informatics, including:
We’ll also discuss information related to:
Applied ethics are standard in most organizations. However, the healthcare industry has a specific branch called bioethics to address the especially critical ethical challenges within health professions. As technology advances and more healthcare systems utilize electronic medical records, the imperative to establish safeguards that ensure compliance with privacy laws and ethical principles grows evermore urgent.
Many ethical considerations arise within health informatics, including patient privacy, information security, transparency in using healthcare data, and preventing bias in the collection and use of information.
Health informatics deals with large amounts of confidential patient information from electronic health records (EHRs), raising many legal issues and ethical concerns. HI must walk the fine line between necessary access to information and protecting patient privacy. We’ll touch on two laws, one being the more important and the other being one of the better known.
The Privacy Act is one of the most important laws that help balance information access and protection. With the advancement of health IT systems, interoperability improves the process of accessing, sharing, and evaluating patient records by physicians, clinicians, pharmacists, and relevant stakeholders on an as-needed and proper basis. Have you ever been curious about how your primary care provider could also view your information from an appointment with a specialist and vice versa? That’s interoperability at work.
Although providers have access to this information, the balance comes from the federal Privacy Act, which protects patients from privacy invasions. ThePrivacy Act includes three key provisions:
The Health Insurance Portability and Accountability Act of 1996 (HIPAA) strengthened privacy protections to prevent the sharing of patient information without knowledge or consent. The U.S. Department of Health and Human Services (HHS) later implemented the HIPAA Privacy Rule, which ensures the protection of an individual’s health information alongside health officials’ right to access information if necessary to protect the public’s health.
As technology advances, so do the information systems that store healthcare data. Big data and machine intelligence are essential tools to help analyze information affecting patient outcomes. Ethical principles for health informatics professionals who access confidential electronic records are equally crucial.
Earlier this year, a team of scholars from the Baylor College of Medicine suggested a new method for patients to control who accesses their information by repurposing nonfungible tokens (NFTs) for the healthcare industry. They proposed that NFT digital contracts could empower patients to specify who accesses and who shares their personal health information. Although this new approach is not in practice just yet due to privacy issues and data security concerns, it proves that technology is ever-changing as it relates to big data and its impact on various industries.
Although patient health data remains confidential, there are instances where individual patient information could influence public health and identify trends. For example, if a physician learns an effective treatment from one patient that could help another patient with similar symptoms, would sharing that information violate that patient’s confidentiality or an imperative act of public health protection? This instance is where transparency becomes critical.
Dr. Kenneth W. Goodman, founder and director of the University of Miami Miller School of Medicine’s Institute for Bioethics and Health Policy, lists three trust-enhancing ways to use the data from EHRs to prevent conflicts of interest and ensure privacy protection:
Another approach to achieving the balance between health information technology and how stakeholders use the data is the Learning Health System (LHS), which originated in the U.S. in 2007. This system has nine core values:
In short, LHSs require the use of secondary health data to help inform decisions that affect public health and shape future patient outcomes while remaining compliant with privacy protections.
Goodman states that “the very nature of machine learning algorithms makes plain that one might unintentionally develop a biased system or accept biased results.” With the rise of artificial intelligence (AI) and algorithms (with machine intelligence doing so much work behind the scenes), it’s still critical to screen output to filter implicit bias to reduce the corruption of health policy.
The Healthcare Information and Management Systems Society (HIMSS) gives the following examples to explain data bias in healthcare even further:
Although AI tools and algorithms populate the data, it is up to the data scientist or informatician to collect, analyze, and use it properly.
The importance of ethics in health informatics is so significant that professional associations like the International Medical Informatics Association (IMIA) expect their members to uphold a standard of ethical conduct. These members include nurses, computer scientists, physicians, and many other professionals who deal with patient confidentiality daily. The ethical guidelines consist of five categories:
The job outlook for health informatics professionals is growing much faster than the overall job market. In addition, as more organizations move toward technology-based platforms to collect, store, maintain, and analyze confidential patient data, the demand for informaticians and additional roles within health informatics to maintain ethical standards should increase.
For example, healthcare organizations must designate a privacy officer to ensure they adhere to federal and state guidelines, investigate privacy violations and concerns, and provide staff training. A privacy officer is just one of many roles to consider in health informatics. Most career paths fall into three categories: analytics, technology, or leadership, with some roles encompassing two or all three skill sets.
A bachelor’s degree in information technology, computer science, or health administration is a gateway into the industry. However, some roles require an advanced degree in specialized areas to move up the ladder and earn a higher salary.
A master’s degree in health informatics opens the door to an impactful healthcare career that doesn’t require years of medical school. Whether you are looking to transition into the field of health informatics or want more knowledge under your belt to excel in a new position, a Master of Science in Health Informatics (MSHI) is perfect for:
If you’re already working full-time, programs like the University of Washington offer a part-time hybrid format. Alternatively, more flexibility is available through a self-paced program like the online MSHI at the University of San Francisco or the online MSHI at the University of Pittsburgh, which has virtual or on-campus learning options. A health informatics master’s degree program can take one to three years to complete; the average time frame is two years of full-time study.
Opportunities to take additional courses within a specialized concentration vary by the program selected and the college or university. Examples include:
There are many options available to build your career in health informatics. In addition, having an advanced degree opens more opportunities to connect big data and medicine without violating ethical principles.
Questions or feedback? Email editor@noodle.com

Industrial engineers use fundamental skills transferable to systems and management [...]

IT professionals are coming out of the woodwork to secure [...]

Many people pursue their master's in industrial engineering to advance [...]

A Master of Science in Industrial Engineering provides expert knowledge [...]
Categorized as: Health Informatics & Sciences, Information Technology & Engineering